Marketing Ideas for Photographers: 26 Strategies for 2026
Discover proven marketing ideas for photographers. Learn strategies to attract dream clients, grow your business, and boost revenue with tactics that work.
AI will not replace radiologists. Instead, AI serves as a powerful augmentation tool that enhances diagnostic accuracy, reduces workload, and addresses workforce shortages while radiologists remain essential for complex decision-making, patient communication, and clinical context interpretation that AI cannot replicate.
Back in 2016, Geoffrey Hinton—a computer scientist who won the Turing Award (and later the Nobel Prize in Physics in 2024)—made a bold prediction that sent shockwaves through the medical community. He claimed training radiologists was pointless because deep learning would surpass them within five years.
It's 2026 now. So what happened?
Radiology didn't collapse. Radiologists didn't vanish. In fact, the opposite occurred. The Bureau of Labor Statistics projects employment in radiology will grow 5 percent from 2024 to 2034, outpacing the average 3 percent growth across all occupations.
Radiology has become the ultimate case study for why AI transforms jobs without eliminating them. The technology handles repetitive tasks brilliantly, but the human expertise behind diagnosis, clinical judgment, and patient care remains irreplaceable.
Here's what's actually happening in radiology departments across healthcare systems today.
Hinton's 2016 statement reflected a common misunderstanding about how AI integrates into clinical workflows. The assumption was simple: if AI could read images accurately, radiologists would become obsolete.
But radiology involves far more than pattern recognition on scans.
According to the American College of Radiology, radiologists face a workforce shortage coupled with growing imaging volume demands. AI hasn't replaced these professionals—it's helping them manage an unmanageable workload.
Data from Indeed provided to CNN indicates there were more radiology jobs in recent years, not fewer. The demand for human radiologists sits at an all-time high.
Real talk: the debate isn't about replacement anymore. It's about collaboration.
The distinction between augmentation and replacement matters tremendously.
Radiology combines digital images, clear benchmarks, and repeatable tasks—exactly the kind of environment where AI excels. But that same environment requires clinical context, patient history integration, and complex decision-making where humans remain superior.
Of the nearly 1,000 AI and machine learning devices the FDA has authorized for healthcare, roughly 75 percent serve purposes in medical imaging. No clinical area has adopted artificial intelligence as quickly as radiology and imaging sciences.
Current AI capabilities include:
Research published in Diagnostics found that an AI triaging system for chest X-rays achieved accuracy of 0.98 (95% CI 0.978–0.988) when validated against radiologist reports. During external validation, the algorithm demonstrated better sensitivity in 6 out of 11 classes than physicians with varying experience levels.
One radiologist at University Hospital described the technology as "kind of like magic" when discussing how AI changes daily practice.
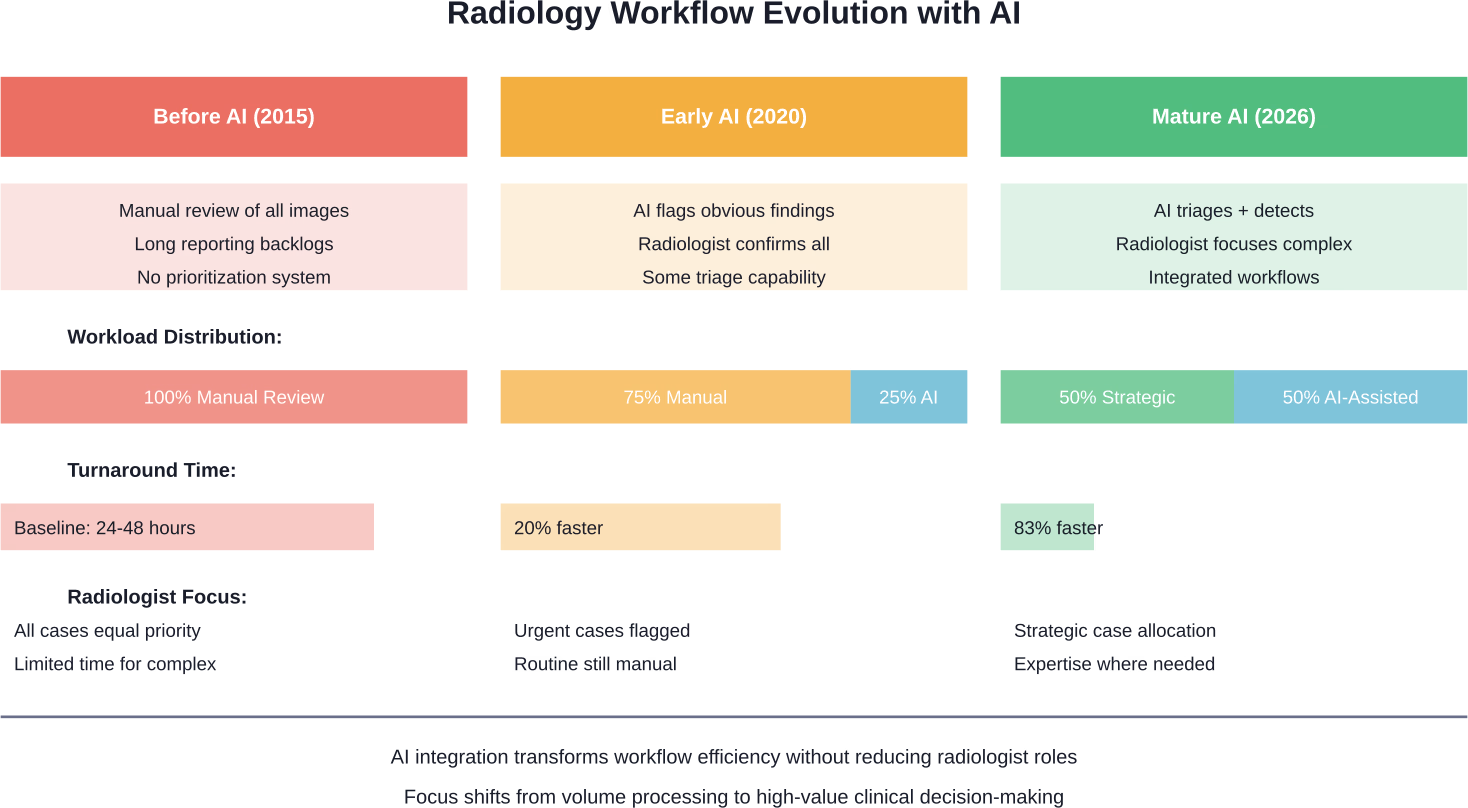
Healthcare centers using validated AI radiology tools report up to 83 percent turnaround time reduction for certain examinations.
Here's where the limitations become crystal clear.
AI struggles with:
Research from the National Institutes of Health examining AI generalizability in radiology found that while models showed remarkable accuracy on institutional datasets, concerns about external performance persisted when encountering different clinical settings.
A systematic review published in Annals of Medicine and Surgery identified six studies addressing diverse diagnostic tasks using deep learning architectures. The research highlighted generalizability as a critical challenge—AI trained at one hospital often underperforms at another.
And here's the thing: radiologists don't just read images. They correlate findings with lab results, consult with treatment teams, perform image-guided procedures, and make judgment calls that algorithms can't replicate.

If AI were truly replacing radiologists, employment numbers would plummet. That's not happening.
The Bureau of Labor Statistics projects total employment to grow from 170.0 million in 2024 to 175.2 million in 2034, an increase of 3.1 percent. Radiology outperforms this average at 5 percent projected growth.
The American College of Radiology identifies workforce shortage and growing demand as critical challenges threatening patient access. Imaging volume continues climbing while radiologist supply struggles to keep pace.
This creates the perfect scenario for AI augmentation. Technology handles volume surges and routine screenings, freeing radiologists for complex cases requiring expert interpretation.
Sound familiar? It mirrors what happened with ATMs and bank tellers.
Repeating periodic concerns raised regarding mechanical technology, some observers in the 1950s and 1960s argued computers and industrial automation could lead to massive job losses. Congressional hearings and studies by the Bureau of Labor Statistics examined these predictions.
The jobs didn't disappear. They transformed.
ATMs automated cash dispensing—a task that consumed significant teller time. Banks responded by opening more branches and shifting tellers toward customer service, sales, and relationship management. Total teller employment remained stable or even grew in many markets.
Radiology follows a similar trajectory. AI automates image analysis components while radiologists shift toward consultation, procedural work, and multidisciplinary care coordination.
Community discussions on platforms like Reddit feature reports from practitioners confirming this shift. Practitioners report AI tools reduce time spent on straightforward cases, allowing more attention for complex patients who need it most.
The practical implementation of AI in radiology looks different from the replacement narrative.
Kevin L. Smith, MD, sees AI changing radiology practice through specific, bounded applications rather than wholesale replacement. At University Hospital, radiologists sit in front of banks of displays with AI assistance running in the background, flagging potential findings for human review.
Diagnostic imaging shows higher maturity than interventional workflows. Research examining AI workflow automation found that 70 percent of MRI and 64 percent of CT steps have available AI solutions, compared to 55 percent in coronary stenting and 36 percent in liver cryoablation.
Not all AI radiology products deliver equivalent value. Clinical validation determines which tools actually improve patient outcomes versus which simply add computational overhead.
The FDA encourages development of innovative, safe, and effective medical devices, including devices that incorporate artificial intelligence. The AI-Enabled Medical Device List tracks authorized products, providing transparency into the current device landscape and regulatory expectations.
Validated systems demonstrate performance across different clinical settings—not just the institution where they were developed. External validation studies test whether algorithms generalize to new patient populations, different imaging equipment, and varied clinical workflows.
A study published in Frontiers in Artificial Intelligence examined clinical validation of an AI algorithm for classifying tuberculosis and pulmonary findings. During external validation utilizing ground truth generated by board-certified thoracic radiologists, the algorithm achieved better sensitivity in 6 out of 11 classes than physicians with varying experience levels.
But here's the critical detail: Group A physicians (more experienced) demonstrated higher agreement with the algorithm in identifying markings in specific lung regions than Group B physicians (37.56% Group A vs. 21.75% Group B). The technology augmented expert performance rather than replacing clinical judgment.
When implemented thoughtfully, AI delivers measurable improvements to radiology workflows.
Research published in the International Journal of Computer Assisted Radiology and Surgery examined workflow automation, accuracy, and efficiency gains. A structured taxonomy distinguished between full automation, human-augmented improvements, and novel AI-enabled guidance functions.
Benefits include:
A large language model extracting findings from radiologist reports achieved accuracy of 0.98 (95% CI 0.978–0.988) when validated against independent radiologist review of a 300-report subset, demonstrating reliable ground truth establishment for training and testing AI systems.
The short answer? AI makes radiologists more effective, not obsolete.
Now, this is where it gets interesting. AI augmentation only works when humans maintain appropriate oversight.
Overreliance creates new risks:
Research on AI generalizability highlights that models encountering data from different hospitals often underperform compared to institutional datasets. Radiologists must recognize these limitations rather than treating AI as infallible.
The American College of Radiology emphasizes strategic deployment of AI tools with patient safety and appropriate reimbursement in mind. Technology should enhance clinical judgment, not replace it.
The people actually using AI in clinical practice offer valuable perspectives.
Community discussions reveal radiologists view AI tools as assistants rather than threats. Practitioners describe faster identification of critical findings, reduced eye strain from prolonged screening sessions, and more time available for challenging cases requiring deep expertise.
But wait. Radiologists also express concerns about overreliance, vendor lock-in, and the need for continuous validation as patient populations shift over time.
One recurring theme: those who use AI effectively will outperform those who don't. The technology creates competitive advantage for practices that integrate it thoughtfully into workflows.
This mirrors broader employment trends. The Bureau of Labor Statistics analysis of technology-impacted occupations found that while technology may disrupt occupations, it won't kill jobs. Adaptation matters more than resistance.
Implementing AI involves costs that must be justified through improved outcomes or efficiency gains.
The American College of Radiology addresses the economics and strategic deployment of AI in radiology, emphasizing patient safety and reimbursement considerations. Institutions must evaluate whether AI tools genuinely add value or simply create additional expenses.
Factors influencing deployment decisions include:
Check official product websites for current pricing on specific AI radiology platforms, as costs and subscription models vary significantly.
The economic case strengthens when AI addresses clear pain points—like emergency department backlogs or subspecialty shortages—rather than automating tasks radiologists already handle efficiently.
The trajectory points toward "islands of automation" rather than wholesale replacement.
Specific tasks within radiology workflows become automated while others remain firmly in human control. AI handles triage, quantification, and first-pass detection. Radiologists handle correlation, communication, procedures, and complex synthesis.
Research examining AI in radiology and interventions found that diagnostic imaging shows higher maturity than interventional workflows, with 70 percent of MRI steps having available AI solutions compared to 55 percent in coronary stenting and 36 percent in liver cryoablation.
This pattern will likely continue. Predictable, repeatable tasks get automated. Variable, context-dependent tasks require human judgment.
The American College of Radiology impact report highlights efforts shaping healthcare policy, advocacy, research, educational offerings, and successful implementation of new technologies. The specialty adapts to AI rather than being displaced by it.
Training programs increasingly incorporate AI literacy into radiology residencies. Tomorrow's radiologists will expect AI assistance as standard practice, similar to how current practitioners expect digital PACS systems rather than film lightboxes.
The skills radiologists need evolve accordingly:
That said, core diagnostic skills remain essential. AI cannot replace the pattern recognition humans develop through years of training and experience with diverse cases.
Look at the data: radiology employment grows despite AI adoption accelerating. The technology creates new possibilities rather than eliminating the profession.
The evidence consistently points in one direction: AI transforms radiology without replacing radiologists.
Geoffrey Hinton's 2016 prediction missed the mark because it oversimplified what radiologists actually do. Image interpretation represents only one component of a multifaceted role involving clinical judgment, patient interaction, procedural skills, and complex decision-making that AI cannot replicate.
Of the nearly 1,000 AI and machine learning devices the FDA has authorized for healthcare, 75 percent serve medical imaging purposes. This massive adoption hasn't decreased radiologist employment—it's coincided with 5 percent projected job growth through 2034.
The American College of Radiology emphasizes strategic deployment with patient safety as the priority. AI addresses workforce shortages and volume growth challenges while radiologists maintain their central role in diagnostic medicine.
What we are seeing instead is a shift toward collaboration: AI working alongside radiologists to make an unmanageable workload manageable, without replacing the expertise that only humans bring to patient care.
Those entering or currently practicing radiology should embrace AI literacy as an essential skill rather than viewing automation as a threat. The technology amplifies human capabilities when deployed thoughtfully, creating opportunities for radiologists to focus on the most challenging and rewarding aspects of their profession.
The future of radiology isn't human versus machine. It's human and machine working together to deliver better patient outcomes than either could achieve alone.
Ready to learn more about AI integration in healthcare? Explore how other medical specialties are adopting artificial intelligence, discover best practices for clinical validation, and understand the regulatory landscape shaping medical AI deployment.